Regulated Secretion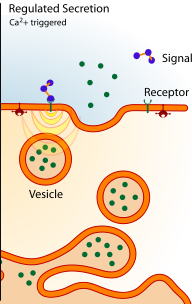
- This pathway occurs only in secretory cells.
- It allows these cells to secrete cell specific products rapidly on demand.
- Secretory products are packaged into vesicles.
- The regulated secretory pathway uses synaptic vesicles and dense core vesicles to store and release secretory products from the cell.
- After their synthesis, vesicles migrate to the site of exocytosis.
- Once a vesicle reaches the plasma membrane, instead of undergoing fusion immediately, they become docked inside the membrane. The vesicles only fuse with the plasma membrane when the cell is stimulated by an extenal signal e.g. ligand binding to a membrane bound receptor.
Image courtesy of https://commons.wikimedia.org/wiki/Image:Exocytosis_types.svg Public domain image.
Functions of the Regulated Secretory Pathway:
1. Release of neurotransmitter from the presynaptic terminal of a neurone.
e.g. muscle contraction caused by the release of acetylcholine at the neuromuscular junction.
An action potential moves down the axon and depolarises the nerve terminal. This depolarisation causes the opening of voltage gated Ca2+ channels in the membrane. Ca2+ flows into the cell down a concentration gradient. The increase in cytosolic Ca2+ levels triggers the release of acetlycholine (ACh) from the presynaptic terminal via exocytosis.
ACh binds to acetylcholine receptors on the postsynaptic membrane (the muscle cell). This causes cation channels to open, resulting in depolarisation of this membrane. A series of events in the muscle cell result in contraction of myofibrils within the cell.
2. Secretion of hormones from endocrine and exocrine glands.
e.g. release of insulin from pancreatic beta cells maintains homeostasis of blood glucose levels.
Insulin is synthesised in pancreatic beta cells and is released into the blood stream by exocytosis on elevation of blood glucose levels. The insulin travels in the blood and binds to insulin receptors found on most cells in the body. This binding stimulates the target cells to increase glucose uptake, via a glucose transporter (GLUT) in the plasma membrane which in turn reduces the levels of blood glucose.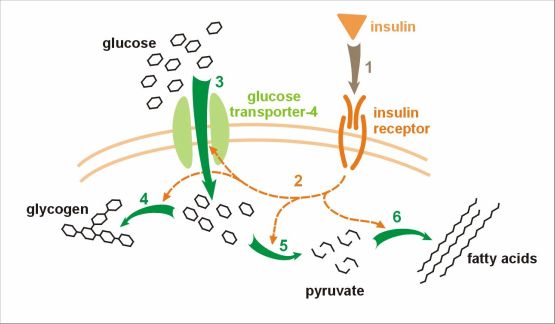
Image courtesy of https://upload.wikimedia.org/wikipedia/commons/8/8c/Insulin_glucose_metabolism.jpg under the terms of the GNU Free Documentation License.
3. Secretion of inflammatory mediators from immune cells.
e.g. release of histamine from mast cells.
Mast cells are cells of the immune system. They are found in most tissues of the body, especially in the skin, digestive tract and mucosa of the lungs. Histamine is synthesised from histidine in a decarboxylation reaction which occurs in the golgi apparatus of mast cells. The mast cells store histamine in dense core vesicles (approximately 3-8pg of histamine per cell). Mast cells are triggered to release histamine during inflammatory or allergic reactions.
When exposed to an allergen (e.g. pollen), specific antibodies (IgE) are produced. Mast cells contain receptors on their surface that bind to the Fc region of this IgE antibody. IgE antibodies bind to these receptors. Mast cells are activated only on second exposure to the allergen. The allergen binds to the IgE antibody on the surface of the mast cell which causes clustering of Fc receptors. This clustering initiates signal transduction resulting in the exocytosis of histamine into the surrounding tissue.
Histamine binds to histamine receptors on target cells initiating various responses depending on cell type. For example, causing contraction of broncial smooth muscle.
Diagram showing histamine secretion from mast cells
Image courtesy of https://commons.wikimedia.org/wiki/File:Histamine.png Public domain image.
